Arizona policymakers have been fighting opioid deaths for several years. They're losing.
The Arizona Opioid Epidemic Act, approved in a special session called by Gov. Doug Ducey in 2018, has led to some successes, but isn't causing a decrease in opioid overdoses and deaths.
When Arizona lawmakers unanimously approved a bundle of new laws in 2018 aimed at decreasing opioid deaths and overdoses, Ducey signed the law in a self-congratulatory press conference and heralded the act as a feather in the cap for bipartisan governance.
But since the Arizona Opioid Epidemic Act passed, overdoses and deaths from opioids have spiked, the state’s own numbers show.
The act largely focused on decreasing legal opioid pill prescriptions from doctors, which was fueling the crisis at the time. But since these laws went into place, more Arizonans are dying from non-prescription opioid overdoses, particularly fentanyl. Some of them, people who work in opioid treatment say, switched from pills to more dangerous street drugs when pills became harder to access.
Public health officials have speculated the pandemic led more people to drugs to cope with pandemic-related stresses using drugs. And their access to care, like medication-assisted treatment, was limited by COVID-19 closures and precautions. Synthetic opioid overdoses have increased across the country, particularly in the West, they note.
But blaming the pandemic for increased overdoses ignores that deaths were already increasing before the pandemic. And pointing to the nationwide rise in opioid overdoses ignores the fact that Arizona policymakers specifically set out to address the problem.
Opioid experts at the state agencies tasked with implementing the act acknowledge the law hasn’t led to the expected reduction in overdoses and deaths, though they say the number of deaths could have been even higher without the legislation.
But as the crisis shifted from legally prescribed medicines — there has been a reduction in opioid prescriptions since the legislation clamped down on the practice — to illicit drugs, the rules of the game for addressing this shift must change, too.

Ducey first declared that Arizona had an opioid-related public health emergency in June 2017, citing figures from 2016 that showed two Arizonans died per day from the drugs.
Now, the number of Arizonans who die per day from opioids is more than double that.
“We're losing five Arizonans a day. We could potentially be losing over 10 a day if naloxone wasn't so readily available throughout the state,” Hazel Alverenga, the deputy assistant director in the Arizona Health Care Cost Containment System’s Division of Grants Administration, said. “So, state overdoses have not decreased at all, but it's in line with the national averages, which are showing increased fatal overdoses across the country.”
The Arizona Public Health Association, an industry group, released a report earlier this year analyzing the act and its effects, saying they “found no evidence to suggest that the epidemic is slowing,” and that drug-related deaths were instead accelerating.
“The data presented in this report indicate that existing intervention efforts (Arizona Opioid Epidemic Act) have not measurably slowed the overall opioid overdose epidemic in Arizona,” the report said. “Further public health intervention efforts and additional resources are needed if the death toll from opioid overdoses is to be reduced.”
The governor’s office acknowledged the crisis has only worsened since the act was passed.
“There are a handful of positive signs, but clearly not enough, given the scope of this problem,” Ducey spokesman C.J. Karamargin said.


The problem was somewhat foreseeable.
Activists at the time warned that the package of laws notably excluded evidence-based measures that have proved effective in reducing opioid overdoses and deaths, like needle exchange programs.
Needle exchanges weren’t initially included because there were mixed feelings among the bipartisan lawmakers working on the legislation, Christina Corieri, Ducey’s senior adviser, said. But since 2018, and as the opioid epidemic has continued to worsen, people’s minds changed, she said.
While needle exchanges were discussed during the 2018 special session, fentanyl test strips didn’t come up at that time, Corieri said.
Lawmakers legalized syringe exchanges and fentanyl test strips this year, though getting ahold of them can be difficult. If those measures were instituted earlier, they could have saved additional lives.
Test strips and needle exchanges are important, Haley Coles, executive director of Sonoran Prevention Works, a harm reduction advocacy group, said. But they’re far from innovative solutions — many states have been offering needle exchanges for decades and fentanyl test strips since fentanyl became a thing.
“We're not particularly special for doing this because this has been proven for decades, all over the world. So I'd really like to see some real innovation,” she said.
Opioid Act targeted pills, but it wasn’t nearly enough
The 2018 opioid act made it harder to prescribe opioids to patients in medical settings. It limited a first fill of opioids to five days, with some exceptions, and put dosage limits in place. It cracked down on “pill mill” doctors who prescribed opioids heavily. It included more education for prescribers and required red caps for opioid pill bottles.
It increased the people who could administer naloxone, and the state has distributed more naloxone since the act was passed. (Any Arizonan can get naloxone at a pharmacy, as the state has a standing order for its use.)
The act also included a $10 million appropriation for treatment programs, including medication-assisted treatment like suboxone or methadone. There’s a Good Samaritan law and an Angel Initiative, where people can drop off drugs to the police and seek treatment. It required electronic prescriptions for drugs that were commonly abused in order to prevent fraudulent paper prescriptions. There were even provisions for veterinarians, in case they suspected a human patient was using the medicines prescribed for their animals.
At the time, Ducey called the act “the most aggressive piece of public policy, the most thorough and thoughtful piece of public policy that’s been introduced in years,” according to a Capitol Media Services story from 2018.

But, even as they were discussing the bills in the 2018 special session, lawmakers questioned why some elements weren’t included and others were. Some called attention to the lack of a needle exchange program, noting the evidence backing up such programs’ ability to prevent other disease outbreaks.
Arizona Sen. Warren Petersen told Capitol Media Services he wondered whether the laws would help at all.
“Whenever government solves problems it doesn’t seem to work out too well,” he told Howie Fischer in 2018. “I hope we’re realizing there are some things government can’t solve.”
Since the initial act passed in 2018, the state created a follow-up plan, with an assortment of tasks designed to address the continuing problem, some with deadlines in mid-2021. Version 2.0 has lofty, specific goals: reduce opioid deaths by 10%, reduce non-fatal opioid overdoses by 15% and reduce overall drug overdose deaths by 10%, all by the end of 2024.
We’ll follow up again at that time, if we’re still around, to see if we meet them. To help us make it to 2024, it’s $7 per month to become a paid subscriber.
And, in the years since the initial special session, the state has added new laws designed to curb opioid deaths and improve access to treatment. In 2019, the state approved a law that allows medical and osteopathic school graduates to automatically qualify to treat opioid use disorder with buprenorphine. And this year, as mentioned, they approved test strips and needle exchanges.
Pills reduced, more access to naloxone — but still more deaths
Despite the spiking number of opioid overdoses and deaths, some measures in the opioid act have proved to be successful, while others are difficult to track or haven’t shown success.
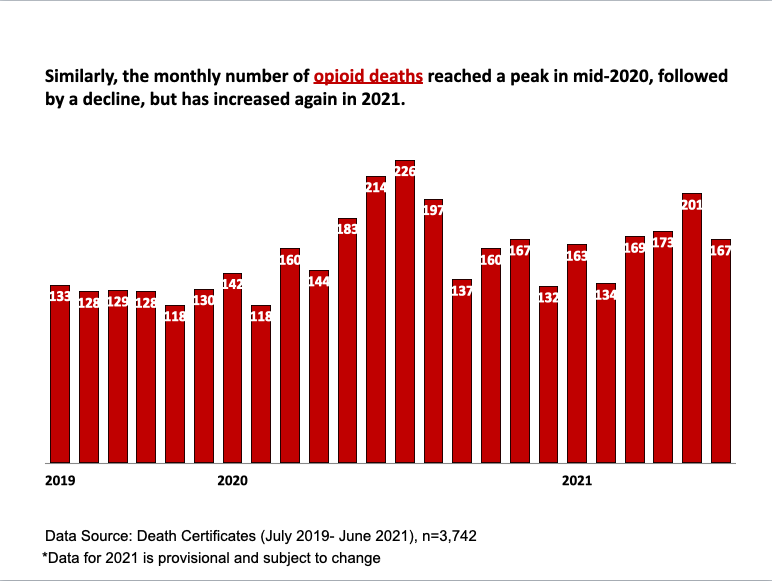
As of now, the peak in opioid overdoses and deaths appears to be mid-2020, though cases decreased after that only to rebound again, numbers from a PowerPoint by the Arizona Department of Health Services in September 2021 shows. Fentanyl and oxycodone were the most common drugs causing overdoses in the last two years.
The number of opioid pills dispensed has decreased by 31% since 2017, the presentation noted. That means fewer people are exposed to opioids in the first place, Sheila Sjolander, Assistant Director in the Division of Public Health - Prevention Services at ADHS, said.
Despite the decrease in pills, though, overdoses have spiked since 2017. As to whether the reduction in pills has played any role in the increased use of illicit opioids, Sjolander said the department doesn’t have any data that would help make that correlation.
“I think we got into a game-changing situation, and it's gonna be difficult to figure out policies to deal with things that are not legally done,” said Don Herrington, the interim director of ADHS.
Coles, of Sonoran Prevention Works, supported the law but said she knew even at the time that the state wasn’t doing enough to actually curb addiction. The law had the unintended but predictable consequence of forcing people to move from prescription drugs to street drugs.
“When you stop people from being able to legally access these medications from their doctors, their pain doesn't go away,” Coles said. “And oftentimes, these doctors don't make an attempt to find alternative pain management for them. Or even if they do, their insurance may not cover it. But people just turn to the streets to treat their pain.”
The same thing happened a decade ago when drug manufacturers were forced to start reformulating pain medications so they couldn’t be injected, she said.
“We just started seeing illicit overdose deaths skyrocket because, again, we're not dealing with the problem,” she said. “We're just making it harder for people to access medications that are a little safer than what you buy on the street.”
The state expected to see improvements within a few years of passing the legislation, but the increase in fentanyl, including in counterfeit and laced drugs, combined with the pandemic, knocked some of the measures off course, Alverenga, of AHCCCS, said. Still, that doesn’t mean there haven’t been successes.
AHCCCS, the state’s Medicaid agency, has seen increased claims for naloxone and substance use disorder treatment since the act passed. For Medicaid members who report they have an opioid use disorder, 30% used medication-assisted treatment in 2017, and that number is now about 60%, Alverenga said.
The act required ADHS to report on gaps in the treatment network, and ongoing quarterly reports show there still are gaps for people who need medication-assisted treatment. A March 2020 quarterly report, for instance, shows hundreds of people who needed inpatient or outpatient treatment for substance use disorder were not able to get it.
More than 130 people were on a waitlist for services during that quarter, the report said, waiting for 38 days on average.
It’s difficult to analyze overall trends in the quarterly surveys, Sjolander said, but the survey does “indicate there's still gaps in the treatment system,” she said.
These gaps are more likely to occur the farther out you get from a metro area, where there’s often a lack of access to all sorts of health care, according to a 2020 report from the University of Arizona.
“The treatment network was not ramped up at the same rate to compensate for the influx of new people who would have a more and more challenging time getting prescribed opioids,” Will Humble, executive director of the Arizona Public Health Association, said.
John Koch, director of community engagement at Community Medical Services, said it’s common to see people using other drugs after not being able to access prescriptions from a doctor anymore.
Community Medical Services, which specializes in medication-assisted treatment, now offers 24/7 treatment at some locations to meet demand and improve access, Koch said.
Corieri said the legislation’s goals were to reduce addictions, increase access to treatment and decrease the number of deaths. The first two were successful, but not the reduction in deaths, she said.
“I think that nobody expected the explosion of fentanyl that came,” Corieri said.
For some other measures, like the red caps on pill bottles, there’s no real way to measure success. The Arizona Board of Pharmacy said there was initially a supply issue for the red caps after the law passed, but that’s been resolved.
“The intent of the Red Caps was to create awareness and we feel it did, however, we cannot determine the misuse use potential decrease,” pharmacy board Executive Director Kam Gandhi said via email.
State still trying to figure out how to prevent opioid deaths successfully
While the first three-plus years of the initial opioid act haven’t worked out as hoped, state health officials say their strategy is geared toward long-term drug prevention. And the increased proliferation of synthetic opioids changed the state’s plans to include more harm reduction strategies, which weren’t initially part of the opioid act.
“We're definitely still in the game, we're still working on this really hard. And we are in it for the long haul,” Sjolander said.
The state has authorization from the Centers for Disease Control and Prevention now to use $100,000 from a federal opioid grant on fentanyl test strips, which will be distributed by partner organizations.
It also recently freed up $1 million from federal funds to buy naloxone nasal spray, though, because of the spiking cost of the drug, that million didn’t buy as much as it could have in past years, Coles said.
This year’s state budget included another $6 million for substance use disorder treatment, Corieri said. Ducey will continue to seek more money for access to treatment, she said.
And AHCCCS has a request for proposals out for a harm reduction program, which could include starting or being a part of a syringe access program. The agency also launched an opioid services locator this week to help people find treatment and naloxone.
The state also launched a new campaign aimed at social connectedness and loneliness, and has another campaign about reducing stigma for seeking substance use disorder treatment.
“It's an ever-moving target. … I think we have new challenges,” Herrington said.
Karamargin, Ducey’s spokesman, said the governor is willing to listen to any other ideas to address the opioid crisis, though wouldn’t say whether the governor had any ideas of his own on that front. Enhanced border security plays a role, Karamargin said, pointing to a recent seizure of fentanyl at the U.S.-Mexico border in Arizona.
“We have further proof that this problem is not going away, and it's not easily solved. Unfortunately, we can't flip a switch,” he said.
Humble, of the public health association, doesn’t think the act was a failure. It slowed down the curve of prescribed opioids. But with fentanyl as the dominant factor now, that requires a different kind of intervention. Cracking down on doctors won’t help. The initial act it could have used more treatment access and harm reduction. Some of the new laws, like fentanyl test strips, make something legal, but still not readily available.
“That's just made it legal. That doesn't mean that you could go into a head shop or a Circle K and buy it. That's what needs to happen,” he said.
Coles agreed that wider access is the first step to ensuring that the latest laws actually reduce opioid deaths and overdoses. But she said truly solving the nation’s drug problems is going to require much bigger thinking.
Some of that would need to be federal policy, like making treatment and medication far more widely available and ensuring insurance covers it. But to solve the real problem, policymakers would have to address the much deeper issues fueling drug use: homelessness, hopelessness and the cycle of crime and poverty that so many users find it hard to break out of.
“My personal belief, and what I've seen repeated in studies, is that the problem that we have right now, it's not just because opioids are available. Drugs have always been available,” she said. “The issue is that we live in a more hopeless, alienating, isolating difficult stratified world.”


